Sept. 23, 2016
Aneurysm survivor says she wasn’t ‘just another patient’ at VCU Health
Share this story
While rushing to retrieve lifesaving equipment for a patient who was gravely ill, Melissa Hurley, a certified nursing assistant, felt sharp pains in her head and neck.
Suddenly, beset by blurred vision and nausea, her face a ghost-white color, Hurley went from someone giving care to someone needing care.
Doctors initially thought Hurley, then 22, might have meningitis. But when spinal fluid from a lumbar puncture procedure produced red fluid instead of clear fluid, she was emergently transported from Fredericksburg to the Virginia Commonwealth University Medical Center Neuroscience Intensive Care Unit.
Her diagnosis? A brain aneurysm, about 5 millimeters by 6 millimeters in size.
Shortly thereafter, Hurley would endure an hourslong surgical procedure called coiling, which restricts blood flow to an aneurysm. She spent 10 days in the hospital.
Less than a year later, the only evidence of the aneurysm is the daily aspirin Hurley takes as a preventative measure. Hurley is back at work and thankful for the care she received at VCU Health.
Considering 40 percent of aneurysm incidences are fatal, brain aneurysm month in September is the perfect time to share her story, she said.
If you have certain symptoms, “don’t wait,” Hurley said. “I only had a headache and blurred vision and I just wanted to go home. I’m glad I didn’t.”
I only had a headache and blurred vision and I just wanted to go home. I’m glad I didn’t.
What is a brain aneurysm?

A brain aneurysm is a weak or thin spot on a blood vessel in the brain that protrudes outward and fills with blood. An aneurysm can press on a nerve or surrounding tissue and burst, which causes blood to spill into surrounding tissues. That is called a hemorrhage. The red fluid doctors drew from Hurley indicated blood was present in her Cerebral Spinal Fluid, which is how they knew the aneurysm had ruptured.
Symptoms of an aneurysm include having a severe headache, changes in your vision or feeling weakness or numbness in your body. Individuals who smoke, have high blood pressure and have a family history of aneurysms are at higher risk. Of those who survive an aneurysm, about 66 percent suffer some permanent, neurological damage.
VCU Health neurosurgeon Dennis Rivet, M.D., was Hurley’s doctor and said her type of full recovery is rare, but she had several things working in her favor.
“Her aneurysm was caught early, it was recognized correctly and she is young and healthy, which adds to her personal and medical resilience,” he said. “Also, she was surrounded by a huge group of people dedicated to helping a person get through this life saving procedure.”
An aneurysm is considered a bleeding stroke, and VCU staff treats 100-150 patients like Hurley each year, Rivet said. In 2015, VCU Medical Center received the first advanced certification as a Comprehensive Stroke Center in Virginia. The certification recognizes hospitals that have state-of-the-art infrastructure and the staff and training to receive and treat patients with the most complex strokes.
“We have a lot of experience taking care of these types of patients,” Rivet said. “We can treat aneurysms through a catheter or an open surgical procedure. Our recommended treatments are individualized for each patient.”
Individualized Care
In recollection of what was her first hospital experience, Hurley says she got careful, thoughtful attention from VCU Medical Center staff.
“[They were] so nice and they didn't make me feel like I was just another patient they had to take care of,” she said. “Dr. Rivet came in every day, talked to me and my family about how things were going, gave us updates and made sure if we had any questions or concerns that he answered them. He made us feel like we were a part of everything, every step of the way. “
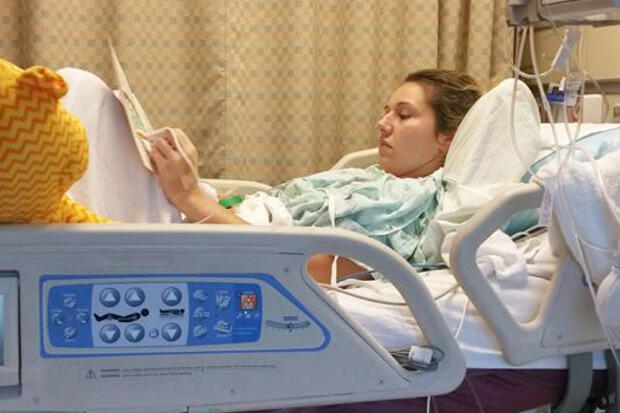
Hurley’s hospital stay involved a slow but steady transition back to good health.
“I was very weak in the beginning so the most they expected from me was to get out of bed and into the [room] chair. By day three I was getting strong enough to walk a little in the hallway and was able to stay in the chair most of the day,” she said. “As time went on I was moved to progressive care from ICU. I was up walking the halls what seemed like every hour.”
Charlotte Gilman is a registered nurse in the Department of Neurosurgery who worked with Hurley as she recuperated.
“I had the pleasure of seeing Melissa progress gradually throughout her hospitalization and then in the outpatient clinic. Melissa made an excellent recovery and recovered quicker than many patients,” she said. “We worked closely together to determine a reasonable return to work plan for her. She was lucky to have a supportive nurse manager [at her place of employment] who allowed her to return to a desk job so that she could get back sooner. I remain involved with Melissa's care as someone she can call for questions about her recovery.”
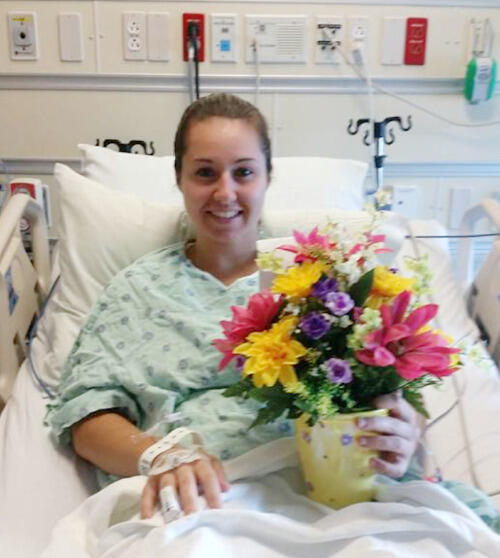
Hurley said she’s glad to be back to her routine, moving forward and free from what she called, “the worst headache I’ve ever had.” She is engaged to be married in October.
“I have no restrictions, but having a brain aneurysm is very scary and it’s something I think about all the time,” she said.
Subscribe for free to the weekly VCU News email newsletter at http://newsletter.news.vcu.edu/ and receive a selection of stories, videos, photos, news clips and event listings in your inbox every Thursday.
Subscribe to VCU News
Subscribe to VCU News at newsletter.vcu.edu and receive a selection of stories, videos, photos, news clips and event listings in your inbox.