Jan. 26, 2021
Here’s what you need to know about the new COVID-19 strains
Share this story
Editor's note: This story originally published on Jan. 19, 2021, and was updated on Jan. 26, 2021, with new information regarding Moderna's tests of its vaccine against the U.K. and South African variants.
As if the world did not have enough to worry about, more contagious strains of COVID-19 are now circulating. A variant originating in the United Kingdom is believed to be twice as contagious and accounts for 60% of the new infections in London, according to the Centers for Disease Control and Prevention. Other variants have come out of South Africa and Brazil. The U.K. variant has been detected in multiple states across the United States, including Virginia.
Michelle Doll, M.D., an assistant professor in the Department of Internal Medicine in the School of Medicine at Virginia Commonwealth University, is a specialist in infectious diseases. Doll talked to VCU News about the implications of the new variants and the means of combating them.
Let’s start by defining terms. Is there a difference between a strain and a variant?
The terms are often used interchangeably, and there is no definite criteria for applying one versus the other on a specific virus. Strains will generally refer to a more established circulating virus, for example influenza B strain, or SARS-CoV 2 being a new strain of coronavirus.
When you are talking about a strain or variant, you are talking about a specific genetic signature of that virus. We know that viruses will mutate over time, steadily accumulating minor changes. Sometimes those changes mean something and sometimes they don’t. If the changes are found to have significance, or the changes begin to vary enough, it is considered to be a different variant or strain. That just means there is something about that version of the virus that is distinct from the parent virus.
Why is the medical community worried about these new strains?
Some of these viral mutations have produced variants with some concerning features. There are changes occurring within the region that helps the virus bind and enter cells. That has implications for not only how it gets into cells, but it also can cause infections and spread. And that has implications for the success of vaccines that are based on the ability to recognize and block that specific interaction.
The variant from the U.K. we seem to know a little more about, because it has been studied a bit longer. The mutation occurs within the spike protein, which is the virus’ binding site for entry into our cells. That mutation has been shown to increase the amount of binding to our cells, and that is one reason it is believed to be more contagious.
Do you get more or less sick?
Scientists studying this variant think you don’t get any sicker than with the most widely circulating virus, but we don’t have enough data yet to be completely sure. Public health experts are keeping a close eye on outcomes of infections with these variants.
How much could this impact the vaccine?
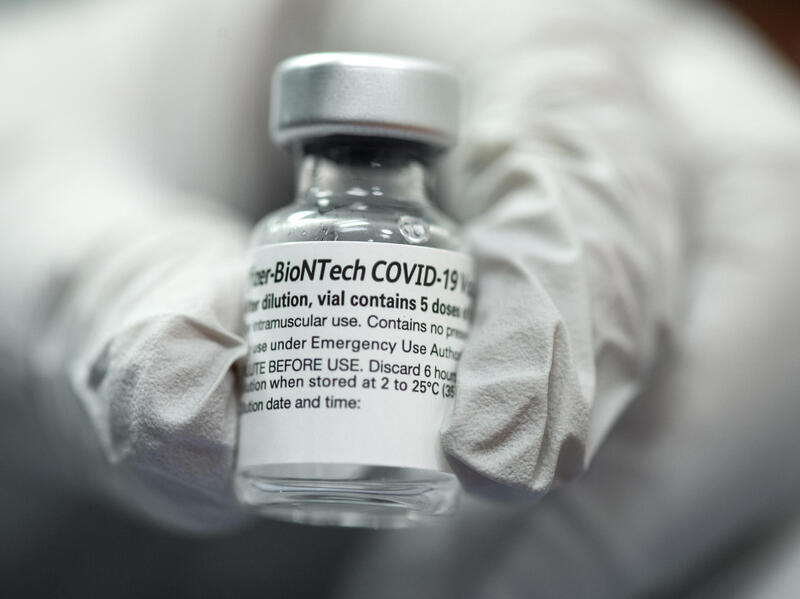
Variant strains capable of escaping our current vaccines’ protection are a concern, but it doesn’t appear that our vaccines are going to be affected by the U.K. variant at the moment. Pfizer published a preprint paper after they studied the specific mutation from the U.K. strain. They put these mutations into the main circulating virus and looked to see if people vaccinated with their product could neutralize it. It did not seem to affect the efficacy of the vaccine.
Moderna recently tested its vaccine product against both the U.K. and the South African variants and found similar good protection from the U.K. variant but potentially less protection from the South African variant. The vaccine is still expected to be protective, but the makers are already anticipating a need to boost the immune response and working on a strategy to accomplish this.
If enough mutations accumulate in our prevailing strain of SARS-CoV 2, we may reach a time down the road where vaccine efficacy is affected. Over time, variants will deviate further and further from the original SARS-CoV 2 strain. It still remains important to get vaccines out as soon as possible and limit community spread through social distancing. In this way, we deprive the virus of opportunities to replicate in new hosts.
Could you have multiple variants in a vaccine?
They are able to incorporate multiple strains into single vaccines. The newer mRNA vaccines can incorporate many different genetic signatures into a single vaccine.
How are the new variants detected?
The way the variant strains are being picked up is with genetic surveillance. They are taking subsets of viral samples recovered from infected persons and sequencing the genetic code. The United States has been criticized for not doing this type of surveillance in a robust way. This was detected in the U.K. in part because of how robust their genetic surveillance is.
Should people take extra precautions because of these new variants?
Now is the time to take extra precautions seriously. But that is not necessarily because of these new variants, but more so because of the surges that we are seeing. The numbers right now are terrible, and I think there is a lot of fatigue with the social distancing and isolation. It’s been hard to avoid activities that we love to do. However, this winter is going to be a vulnerable time with hospitals potentially getting very full. The precautions necessary to combat these variant strains are the same you have been hearing about for months: hand washing, masking, social distancing.
Will the surge in COVID-19 cases continue to be a problem this winter?
It is thought that the surge will continue to worsen through the winter months. There are a lot of theories as to why viral respiratory infections in general surge in cold months. One is that we are inside more. We are closer together, and we potentially gathered together at recent holidays such as Thanksgiving, Christmas and New Year’s.
In addition, in colder regions of the country you have some drying out of the nasal mucus membranes, and potentially viruses have easier access. This virus appears to be more susceptible to humidity, so it may be able to persist longer on surfaces under drier environmental conditions.
We probably will not achieve sufficient vaccination rates across the population to provide a good level of herd immunity [this] winter, though our vaccination programs are certainly trying.
How much should people continue to wash surfaces, or is the virus spread primarily through the air?
I think there probably is a surface component based on what we see from other respiratory viruses. Surface environments are important for our infection control practices.
But there is a bigger component of droplet spread even from normal speech and talking that I don’t think was appreciated at the beginning of the outbreak; certainly the critical intervention of masking has made a big difference in prevention of short-distance droplet-mediated spread.
The challenge with contact spread is that it is pretty much invisible because it is harder to identify and trace those lines of transmission. I definitely recommend diligent washing of your hands.
Have protocols at VCU changed at all given the new variants?
No, we continue to follow the same protocols that we have followed throughout the pandemic. This is still COVID-19, with the same mechanisms of transmission. Our cleaning protocols are the same.
Have either of the new variants been discovered in Virginia?
I would not be terribly surprised if it’s here, but I’m not aware of that being reported. Neighboring states such as Maryland have confirmed cases with the U.K.-variant, so it is very likely we have it in Virginia as well.
Were these variants something that was expected?
Yes, viruses are known to mutate over time, and variations of this particular virus is something that researchers have been discussing throughout the pandemic. Certainly, it has been on the radar of virologists and other scientists working on our vaccines. These researchers are now working to determine the impact to the vaccine these mutations are going to cause. At some point, they might even need to make slight tweaks to the vaccine to maintain good protection.
Do they know if the virus mutates more slowly or quickly in comparison to other viruses?
I am not sure that is known at this point. There has been a suggestion that it actually replicates fairly slowly given that most samples remain essentially unchanged from the main strain discovered in Wuhan, China.
Mutation rates may also be influenced by the intensity of viral circulation. Because mutations occur during interactions with host cells and the host immune system, more host-viral interactions give a virus more opportunity to mutate, and eventually more of a chance that a mutation benefiting the virus in some way will develop and prosper.
Is there still a lot of reluctance to get the vaccine?
The public does seem to have a lot of reluctance around this vaccine in particular. In fairness, the mRNA vaccines are new, developed very quickly in comparison to prior vaccines, and this, along with our current political climate, makes some very nervous.
However, I have seen so many patients die of COVID-19 since [the start of the pandemic] … . Many of these victims were patients who would not otherwise be dead. In other words, they did not have devastating or otherwise terminal underlying conditions. I want to be clear that the imminent risk of COVID-19 is very, very real. Furthermore, some recovered patients continue to have debilitating symptoms long after COVID-19 is gone, and it is unclear at this time if they will fully recover.
My hope is that as we are seeing more and more people vaccinated and we further demonstrate that this is safe and effective, it will help more of those who are nervous make the decision to get vaccinated. Once they see their co-workers and people in their community getting vaccinated and doing well, they will hopefully be more comfortable with getting it themselves.
Subscribe to VCU News
Subscribe to VCU News at newsletter.vcu.edu and receive a selection of stories, videos, photos, news clips and event listings in your inbox.