May 2, 2018
Ultrasound technology can help paramedics save lives in the field. A groundbreaking new class at VCU is training them how.
The course — the first of its kind in the country — is training EMS personnel how to incorporate ultrasound technology into their work saving lives.
Share this story
A 62-year-old male has collapsed on a treadmill at the gym. First responders arrive to find that he’s unconscious and without a pulse. They start CPR.
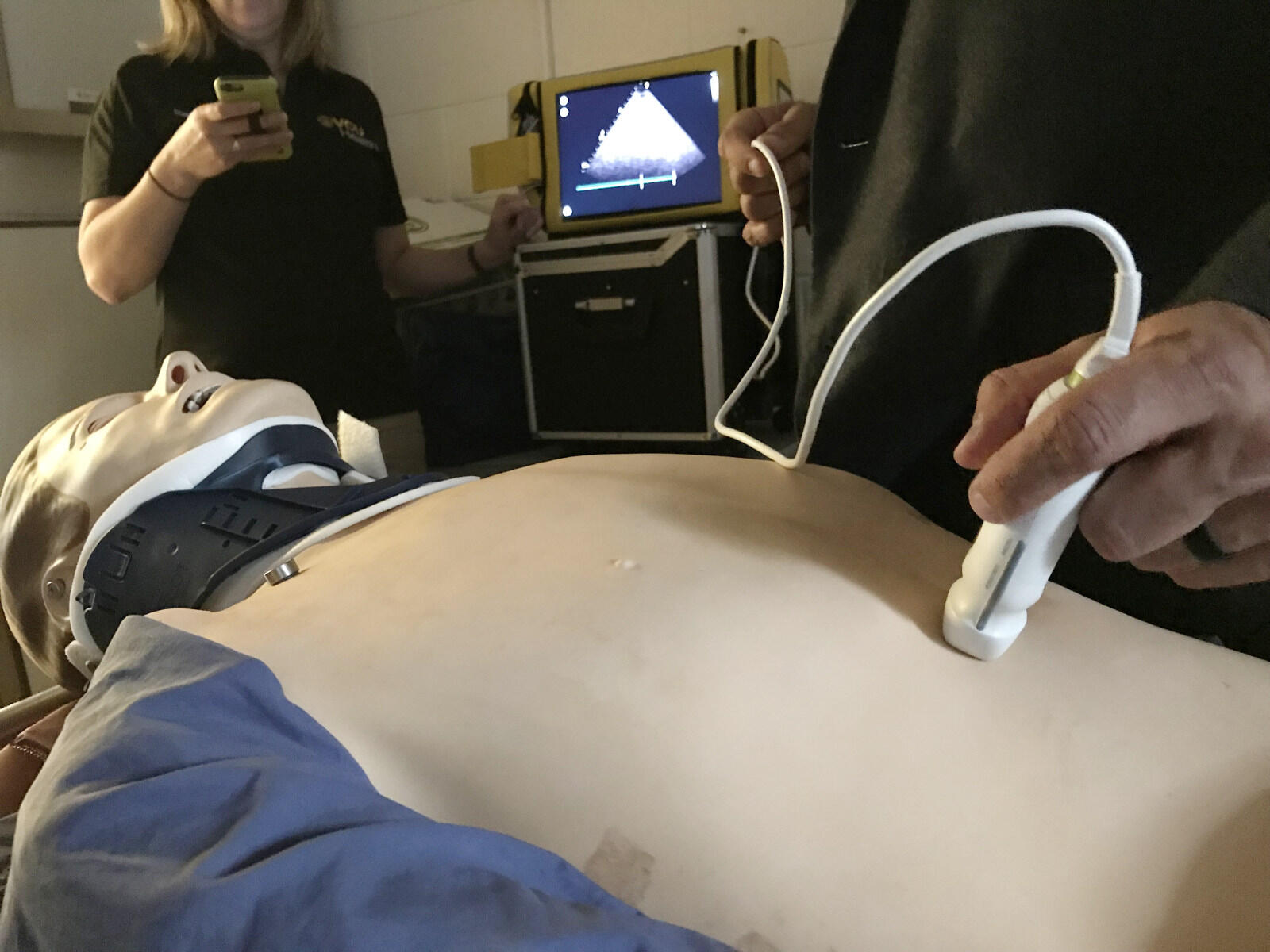
“Let’s see what’ve got,” says paramedic Shawn Lawrence, as he runs a small ultrasound probe over the man’s chest, conjuring up a black-and-white image of the heart on a handheld monitor.
The ultrasound reveals the heart is quivering, just slightly.
“OK, so what do you think?” asks Stephanie K. Louka, M.D., an emergency medical services fellow and clinical instructor in the Department of Emergency Medicine of the Virginia Commonwealth University School of Medicine.
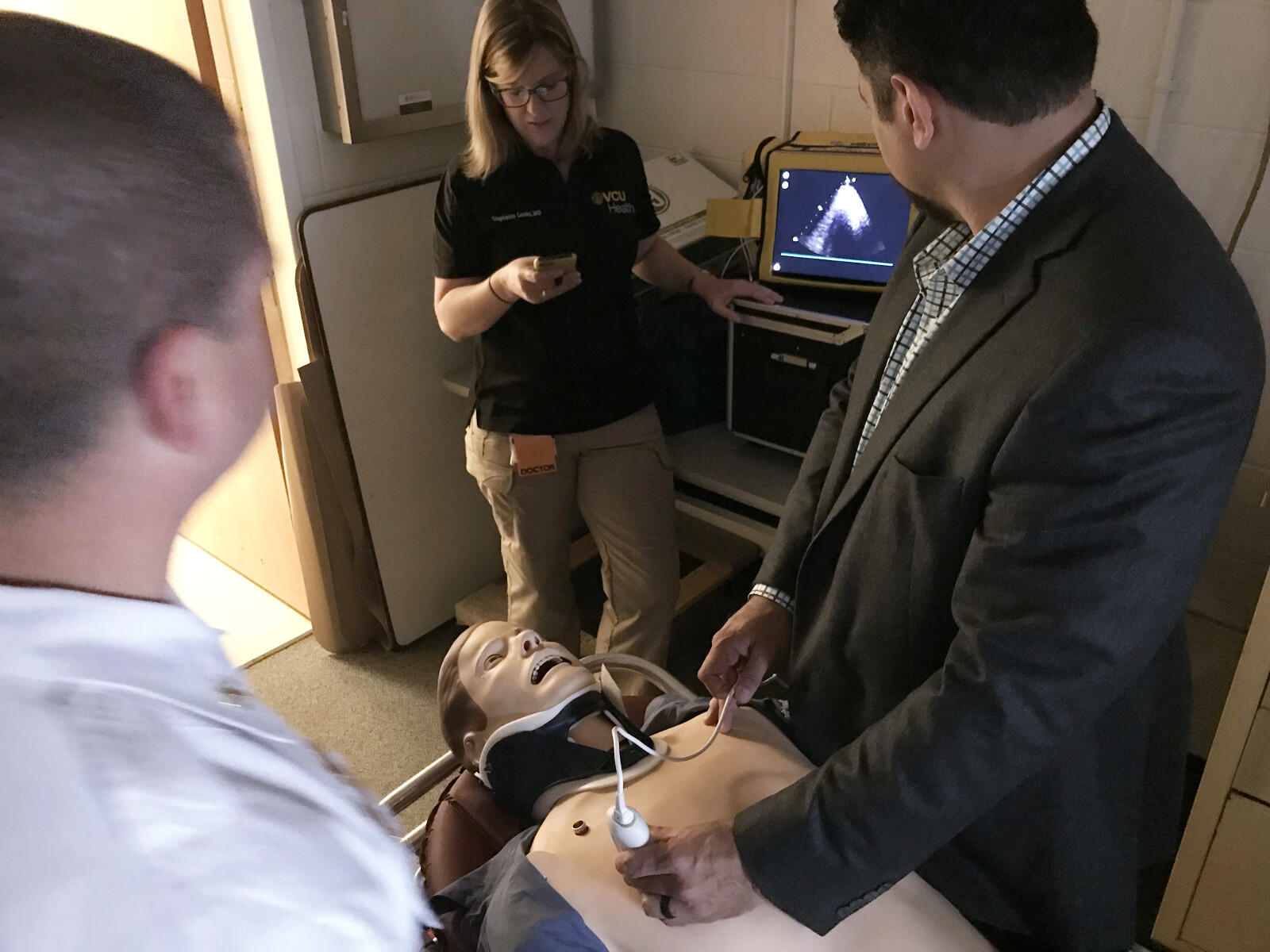
“So, we’re going to shock him,” Lawrence replies. He applies a defibrillator. The ultrasound shows the man’s heart has started beating again with an organized rhythm.
“Oh, I'm happy with that,” Lawrence says. “It looks good.”
This scenario — a simulation in which Lawrence was resuscitating a medical training mannequin — took place in VCU’s trauma skills classroom as part of a new course in which first responder medical personnel from across Virginia are getting hands-on training to use ultrasound technology before the patient reaches a hospital.
“Ultrasound is a more advanced tool for our EMS toolbox,” said Lawrence, a paramedic at Parham Doctors’ Hospital, who is taking the course. “With ultrasound, we can actually see the heart, as opposed to an [electrocardiogram]. Here, we can see the actual mechanical function of the heart. Is it beating or not beating?”
The class is the first in the country in which emergency medicine physicians are training EMS personnel on how to incorporate ultrasound technology, whether in the back of an ambulance, aboard a helicopter or in the field.
“People have called ultrasound the new stethoscope,” said Louka, who is teaching the course. “I think that's pretty fair because with a stethoscope, if you listen to lungs and you hear normal lungs or wet lungs, that gives you information. It's a decision point on how you're going to treat a patient. Am I going to turn left or right in treatment of this patient?
“It’s the same with ultrasound,” she said. “It’s a diagnostic tool that’s small, affordable and very versatile in an environment where you don't have the luxury to have a lot of tools. You can only fit so much into an ambulance, or especially a helicopter. And so, if you consider ultrasound’s versatility, its cost point and the amount of impact you can make, it has a very, very high value.”
Cost, size of ultrasound dropping
The cost and size of ultrasound technology has dropped significantly in recent years, prompting EMS agencies to investigate the feasibility of adding it to emergency transport.
“In the past, ultrasound was cost prohibitive in the pre-hospital environment,” said Basil Asay, assistant director of the VCU Center for Trauma and Critical Care Education. “The one we’re using [today in class] is about $8,000 roughly and it's coming down because of competition. And they have a new one coming to market later this year, and it will actually hook up to any iPhone 6 or greater. At $2,000 it could be a game changer.”
Last year, physicians from the VCU Department of Emergency Medicine trained paramedics with the Richmond Volunteer Rescue Squad on pre-hospital ultrasound. The squad was among the first in Virginia to start carrying ultrasound technology in their ambulances.
VCU LifeEvac also added ultrasound aboard its medical transport helicopters about a year and a half ago.
“Traditionally, money and the size of the technology had been a barrier,” Louka said. “Now that barrier is coming down and EMS agencies are like, ‘Wait, who has the expertise to teach us?’ And that is where VCU identified a need and created this course.”
The course, which is taught by physicians from VCU’s Department of Emergency Medicine, is being offered through the Center for Trauma and Critical Care Education, which was established in 1980 to provide education to Central Virginia’s volunteer EMS community and today provides a variety of comprehensive training programs for medical center and community care providers.
Enrolled in the ultrasound class are paramedics, nurses, flight nurses, nurse practitioners and a physician.
Jeff Powell, assistant chief of the Henrico County Division of Fire, took the class because his agency is considering adopting ultrasound.
“We're certainly interested in looking at all the new trends and techniques in pre-hospital emergency medicine and ultrasound has a lot of promise for a wide variety of patients. It's definitely something we're looking closely at,” he said. “We're trying to be on the cutting edge, learn about ultrasound and take that knowledge back to our department.”
Jason Welch, M.D., an EMS physician and medical director of Operational Medicine Consultants, is also in the class. His company works with private EMS agencies, some of which have already purchased, or are considering purchasing, ultrasound devices.
“I came here to learn about ultrasound and to be able to go on to tell the guys I work with about it and spread it to them,” Welch said. “[It’s valuable because of its] ability to do point-of-care testing. To be able to see, in detail, exactly what's going on inside the body without being invasive, without doing harm to the patient.
“Getting this level of detail, I want to be able to do that,” he said. “And I want the guys that I work with to be able to do that.”
Blanton Marchese, a paramedic and CEO of Emergency Services Solutions, which provides EMS personnel to Powhatan, Amelia, Cumberland and Middlesex, said ultrasound would be a great tool for EMS in rural counties.
“It’ll help improve the decision making and cut down on the time for decisive care,” he said. “It’ll speed up the decision tree on patients with time-sensitive emergencies. This is really going to allow us to bring the care team together much quicker, with more information, and build on a focused treatment plan much earlier.”
A valuable tool in the field

Ultrasound is useful in a number of situations that EMS personnel encounter on a regular basis, most notably cardiac arrest.
“When someone is in cardiac arrest, we can use ultrasound to look at the heart. Sometimes you may not feel a pulse and you may or may not see something on the EKG, the electrical monitor,” Louka said. “Sometimes it's just hard for [the EKG] to pick up something that's really going on. So, with ultrasound, we can actually look and see: Has the heart really stopped? Or is it quivering, in which case we can do something about it?”
If the ultrasound shows that resuscitation is impossible, it reduces the chance of accidents occurring during the ambulance’s high-risk, lights-and-sirens rush to the hospital.
“That is actually one of the very highest high-risk times for an ambulance to get in an accident, and is the leading cause of injury deaths in our profession,” Louka said. “So there's a big public safety risk.”
Ultrasound also can assist paramedics responding to patients who have sustained traumatic injuries.
“We use ultrasound to look in certain spots of the chest, around the heart, in the abdomen to look for fluid, which, in trauma, it's going to be blood — and if we see that and especially if somebody has unstable vital signs, we know that they are definitely going to need to go to a trauma center if not potentially go straight to the operating room,” Louka said.
It can also help paramedics decide the most appropriate hospital to which they should transport a patient.
For example, if the ultrasound shows that a woman with abdominal pain is pregnant they might take her directly to an obstetrics center. Or if paramedics are concerned a patient is experiencing a major myocardial infarction, they can check the ultrasound and decide to go straight to a percutaneous coronary intervention center.
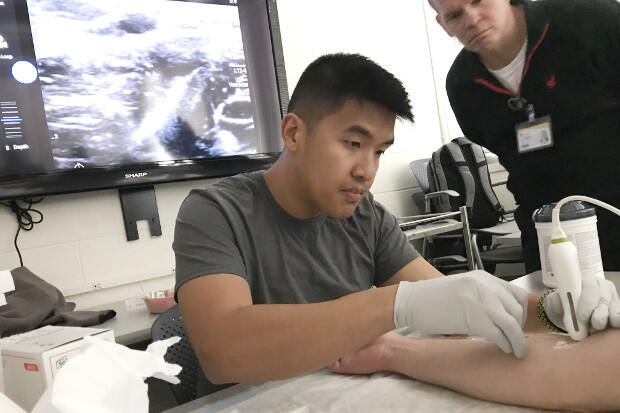
Ultrasound can also be a helpful tool for paramedics to easily find veins and avoid arteries when inserting an IV.
“It helps you find the right pipe,” said Michael Ny, a firefighter and paramedic in Chesterfield County.
Ny, who took the class just to better understand an up-and-coming tool in pre-hospital care, was initially a bit skeptical.
“I came in thinking, I work for a jurisdiction that's very close to the hospital. How could this be of any benefit? I've been practicing for the last almost five years and have never had the need for an ultrasound. So why now?
“But much to my surprise, in this class I've been able to learn a lot of applications for ultrasound that we can use as pre-hospital care providers,” he said. “We've seen how ultrasound can be a really amazing, quick diagnostic intervention.”
Subscribe to VCU News
Subscribe to VCU News at newsletter.vcu.edu and receive a selection of stories, videos, photos, news clips and event listings in your inbox.