
Nov. 15, 2017
Father and son, treated for burn injuries 48 years apart, emphasize the personal side of patient care
Share this story
It was a typical Saturday morning in 1963 for Robert Langhorne. And then, it wasn’t.
Langhorne was standing in the yard outside his Cumberland, Virginia home, trying to destroy leftover blasting powder he’d poured in the grass. He’d been using the blasting powder to destroy firewood in his yard. After several failed attempts to disintegrate the blasting powder with fire, the substance suddenly ignited and flames shot upward and engulfed his face. Langhorne ran into his home and pulled his T-shirt up and over his head to remove it, which peeled the burned flesh from his face.
“What in the world has happened,” he remembers thinking.
His family drove him about eight miles to the nearest rescue squad. First responders transported him to Virginia Commonwealth University Medical Center for treatment. Langhorne stayed in the hospital’s burn unit, now the VCU Health Evans-Haynes Burn Center, for almost two weeks and experienced a full recovery without disfigurement to his face. He remembers, “They made me feel like I was at home. They were kind and listened.”

Almost a half-century later, on March 2, 2011, Langhorne found himself in a similar situation. But this time, he was the one summoning help for a family member. He and his son, Terry, were trying to start a vintage, red, 1976 Chevrolet Monte Carlo in a garage when flames burst from the hood. Terry Langhorne suffered fourth-degree burns on his face, chest and arms. In that moment, Robert Langhorne’s memory and sentiment for the Burn Center returned, vividly. And because of the superb treatment he received nearly 50 years earlier, he was adamant his only living son be transported from Cumberland to the very same center that treated him. Terry Langhorne spent several weeks in the intensive care unit, but survived and is now doing well.

“I thought, ‘If Virginia Commonwealth Medical Center can’t help you, nobody can help you,’” said Robert Langhorne, now 74. “It brought back memories you try to forget. A lot of memories I can’t forget now. But [my son] surviving is the best part of it and VCU Medical Center played a big part in that.”
As the Burn Center celebrates its 70th anniversary this year, stories such as the Langhornes’ magnify the uniqueness of the center. The Burn Center is the oldest civilian burn facility in the country, and yet it is also equipped to handle the 21st-century needs of burn patients.
“We want to remain on the cusp of burn care. That means state-of-the-art surgical options, research on using artificial skin [for skin grafts] and ongoing research relative to treating burn patients,” said Michael Feldman, M.D., Evans-Haynes’ medical director. “I see us being a leader in the community for burn prevention and education.”

In a class by itself
The Burn Center is a 16-bed space with an eight-bed ICU, eight non-acute beds, and treats between 400 and 450 patients annually. Patients with acute burns, as well as those with reconstructive needs or those who have been injured by fire, chemical scalds and electrical burns are treated in the Burn Center. In July, the Burn Center received its reverification as an adult and pediatric burn center by the American Burn Association. VCU Medical Center is the only Level I trauma center in the state verified by both the American College of Surgeons as a Level I adult and pediatric trauma center, and by the American Burn Association as a Level I adult and pediatric burn center. Andrea Pozez, M.D., professor and chair of the Division of Plastic and Reconstructive Surgery, has been at Evans-Haynes for 30 years and remembers when offerings weren’t as sophisticated. Division of Plastic and Reconstructive Surgery faculty, who are trained in the management of burn injuries, provide patient care in the Evans-Haynes Burn Center.
“We started out as a smaller entity with individuals taking care of patients,” she said. “Over time, we’ve transitioned into multidisciplinary care of patients. Our most significant enhancement has been having patients’ families present and making them comfortable and part of the patient’s recovery. Patient outcomes are much better because of that.”
As part of patients’ care, psychologists, nutritionists, rehabilitative specialists, dietitians, social workers and pain specialists are available if necessary. Involving patient families and various health disciplines makes for a better patient transition, Pozez said.
“We can help them manage their long-term recovery,” she said.
Part of the Burn Center’s reverification designation came with commendations for strong administrative and multidisciplinary support, strong community education programs, and a vigorous nursing burn competency program.
Tiffany Lord was part of the behind-the-scenes process to help the Burn Center obtain its reverification this summer. She has worked as a nurse clinician there for three years and said it was hard to encapsulate on paper what staff does so seamlessly for patients. Still, it was worth it.
“It’s just our day-to-day job, but when you look at it on paper it’s exceptional what we do,” she said. “This allows the community to see we’re committed to our patients.”
Safety first
The Burn Center has a longstanding footprint in the community, particularly with its yearly Burn Survivor Sunday event. For the past 20 years, the event has been a chance for burn survivors treated at VCU Medical Center to share their stories and reconnect with staff who treated them. It’s also an opportunity to recognize first responders throughout the Richmond area who initially treat and transport patients. In October, as part of a VCU Health occupational safety fair, Burn Center staff made available materials about home fires and smoking safety, and offered demonstrations on how to prevent and react to kitchen fires.
Educating the community is as important as treating patients, said Wendy Lugo, nurse manager for the Burn Center.
“As much as we can we want to prevent someone from becoming a burn victim,” she said.
The student community also does its part to support the Burn Center. For the past six years VCU’s Pi Kappa Alpha fraternity has raised more than $100,000 for Evans-Haynes through its annual Fireman’s Challenge, which raises money to support burn staff training, burn rehabilitation equipment and toys for youth patients. The event is PIKE’s annual philanthropic effort to benefit and raise awareness for Evans-Haynes and began after a VCU student took a tour of the facility and was inspired to do more to help patients.
The work done at the Burn Center is motivating, not only to outsiders but also to those working within. Brian Le, M.D., is an assistant professor of plastic surgery within the Division of Plastic and Reconstructive Surgery. He was an undergraduate medical student at VCU from 2005–09 and said training under the current faculty inspired him throughout his studies.
“I’ve seen so many of my mentors who will go out of their way to bring patients their favorite food after they’ve been [taken off] NPO [nothing by mouth],” he said. “Dr. Pozez, the way she interacts with patients is magical — the care, the gentle voice, the nurturing. This is a great place to train or to work.”
Jeffrey Haynes, M.D., is a professor of surgery and pediatrics and director of the Children’s Trauma Center at Children’s Hospital of Richmond at VCU. CHoR is the only ACS-verified Level I pediatric trauma center in the state. The severity of a child’s burn injury will determine whether they are initially treated by Haynes’ team at CHoR or at the Burn Center. A trip to the latter likely indicates they were treated emergently and seen as an outpatient. More specific, long-term pediatric care is available at CHoR after a child is initially diagnosed.
The tag-team approach of caring for a burned child is unique, Haynes said.
“The Evans-Haynes Burn Center is a very important partner with us in the Children’s Trauma Center. We offer a resource through south-central Virginia and beyond, for any injured child,” he said. “We pride ourselves in total preparedness and being able to provide for any child, in any shape, who needs help.”

Right: Dr. B.W. Haynes was director of the Burn Center for 36 years.
CHoR’s team includes a full scope of pediatric subspecialties to care for trauma and burn patients, including neurosurgery and orthopedic physicians working within a pediatric emergency room and a pediatric ICU. CHoR also has pediatric equipment specifically sized to treat children. The depth of the hospital’s pediatric offerings sometimes surprises Haynes, who is the son of B.W. Haynes, M.D., the latter half of the Burn Center’s namesake. It is rewarding to honor his father’s vision and long term medical direction, Jeffrey Haynes said. B.W. Haynes was medical director of the Burn Center from 1954 to 1991, after the death of the Burn Center’s founder Everett I. Evans, M.D.
“I am still a little bit amazed at how well the system works, how well we can bring all these consultants together and the child is there and beautifully taken care of,” he said. “All the consultants put their plan in and it all sort of [works] out to be one great treatment plan where everyone works together. We have all these partners … including the Evans-Haynes Burn Center.”
‘Painwise, the technology and the doctors were so good’
Terry Langhorne has fond memories of the team who helped him during his two-month stay at the Burn Center, and particularly Feldman.
“He’s an awesome man. Whatever I had for him, he had an answer for and if he didn’t know, he’d try to find out for me,” he said. “The whole staff was good. We had a pretty good relationship.”

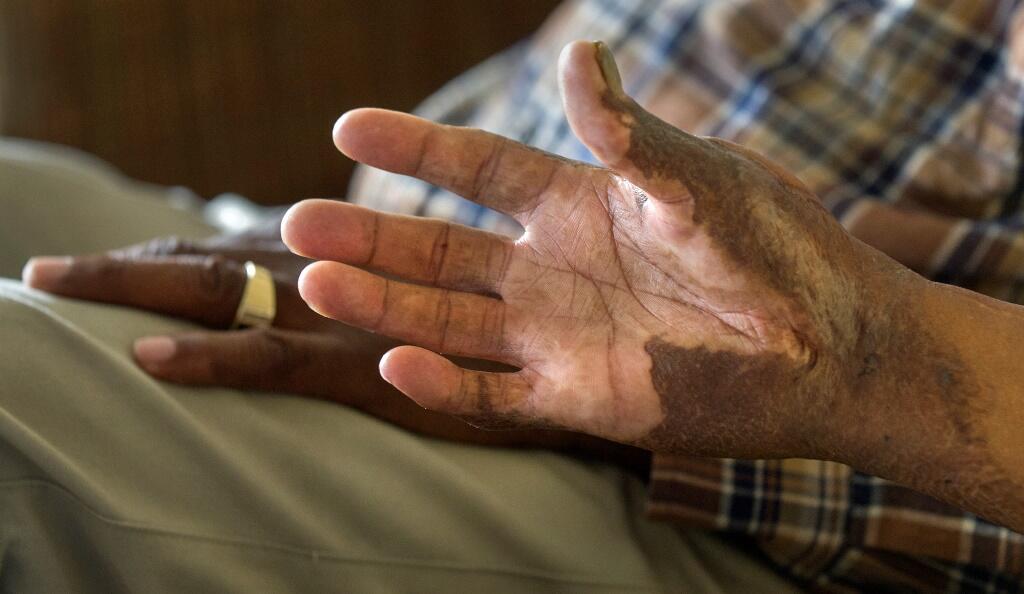
Terry Langhorne, now 55, was sedated for one of the two months he spent at the Burn Center. He had seven skin graft surgeries, and all of the fingers on his left hand were amputated in order to save the arm. Like his father so many years ago, when he was first burned, Terry Langhorne said he didn’t know what was happening.
“It wasn’t clear to me that I was on fire,” he said. “I wasn’t in pain, but I could feel something itching. My jacket was on fire. My father was telling me to take my jacket off and then I fell to the ground.”
Terry Langhorne’s memory returns around about the time he started to consciously experience his recovery. Surprisingly, he remembers his discomfort being mild then, too.
“Painwise, the technology and the doctors were so good, they limited the pain even with all I went through,” Terry Langhorne said.
The Burn Center will continue to evolve with a combination of state-of-the-art equipment and dedicated, compassionate staff. Faculty are currently studying a technique to create artificial skin, tissue engineering, which would reduce the number of skin graft surgeries a burn victim would need to endure during recovery.
Experiences like those of the Langhorne family keep Feldman and his team focused on outreach and the next steps in the field of burn care. Feldman distinctly remembers Terry Langhorne’s case and the severity of his issues. He uses that memory as motivation.
“He had some of the worst burns I’ve seen,” Feldman said. “He had fourth-degree burns, which means the burn has gone through all your layers of skin in addition to going down to muscle, tendon and bone. There were surgeries to reconstruct his mouth and his right hand to improve function. I rave about him. He’s so inspirational to anyone who says ‘I just can’t do it.’ You have to look at Terry and think anything is possible.”
For the next 70 years, the Burn Center will focus on casting a wider net around those they can help.
“We’re looking to branch out not just with local care, but nationwide,” Feldman said. “We want to help the entire United States treat more burn patients, which even includes mass casualty incidents.”
Terry and Robert Langhorne are grateful for the Burn Center’s enduring commitment to burn care.
“Not too many people know how important it is to have someone that can help you,” Terry Langhorne said. “I didn’t have a clue where to go. But it’s a good thing my father did.”
Subscribe to VCU News
Subscribe to VCU News at newsletter.vcu.edu and receive a selection of stories, videos, photos, news clips and event listings in your inbox.








