
March 28, 2013
Medical students learn art of patient perspective
Share this story
A well-known Native-American proverb says, “Tell me and I’ll forget. Show me, and I may not remember. Involve me, and I’ll understand.” That principle serves as a cornerstone of the new medical school curriculum at Virginia Commonwealth University, where hands-on, active-learning reigns.
In recent years, simulation-based education has become a growing trend in medical schools across the country, and the VCU School of Medicine has been among the frontrunners.
As it launches a new medical school curriculum focused on active-learning, VCU aims to help these future physicians learn to practice medicine efficiently and with empathy and caring through a unique collaboration between the VCU School of Medicine and the VCU School of the Arts.
VCU’s Standardized Patient Program is designed to help medical students learn to effectively conduct the physicians’ traditional interview: the history and physical. They will learn to care for the entire spectrum of the patient population – from pediatric to geriatric patients.
Traditionally, medical students’ first encounters with patients occur when they begin training on the hospital’s different units with faculty physicians. Now, however, students will work with standardized patients from the first day of medical school. These individuals are trained to act as patients and to participate in active role-playing with medical school students.
The standardized patients are taught to give feedback to the students and are familiar with steps involved in taking a patient’s history and performing physical examinations. For example, these specially trained patients can tell the medical student whether he or she has palpated the abdomen hard enough to feel the liver.
“Sometimes learning involves very sick patients, or very invasive procedures. In those cases we use high fidelity manikins and their sophisticated software,” said Ellen L. Brock, M.D., medical director of the VCU Center for Human Simulation and Patient Safety, which is home to the Standardized Patient Program.
“Sometimes learning involves developing communication skills, the ability to take an accurate medical history and becoming comfortable with the physician/patient human interaction. This is where our Standardized Patient program makes such a dramatic contribution,” she said.
“What inspires me about this work is that when art is used in health care the impact can be both direct and profound,” said Aaron Anderson, Ph.D., associate professor and associate chair of the Department of Theatre in the VCU School of the Arts, who has played a key role in launching the program at VCU.
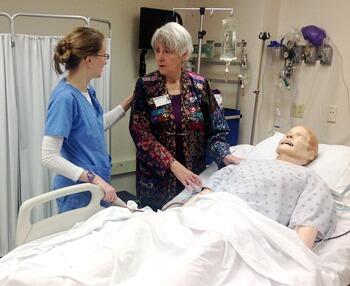
The power of simulation-based education
The VCU Center for Human Simulation and Patient Safety provides simulation-based training for faculty and medical students of the School of Medicine and for trainees and staff of the VCU Health System. The center is located in the new James W. and Frances G. McGlothlin Medical Education Center, and has approximately 25,000-square-feet of simulation space equipped with state-of-the-art simulation technology. Physician groups from outside VCU also are expected to visit to learn new techniques in surgery or treating critical care patients.
“Simulation represents the difference between learning about something and learning to do something,” said Brock.
“It is the place where students apply theoretical and abstract knowledge to a concrete environment. It allows learners to practice the skills necessary for excellent clinical performance before they use those skills on real patients. And it allows reflection on that performance, and identifying and testing opportunities for improvement – with technical, cognitive or teamwork skills.”
The newly-designed space houses a tremendous variety of simulation, a simulated operating room, ICU and more. It also has an entire floor dedicated to 14 patient rooms for the Standardized Patient Program that are equipped with hand-washing sinks, exam tables and patient gowns. There is an area for the student to sit down and take notes at the computer where they can assess a patient case, work through the process of a differential diagnosis to determine what is ailing a patient and develop a treatment plan.
As students go through the first three months of the curriculum, they’ll be working in the simulation rooms. Interactions of the medical students with the standardized patients will be recorded and faculty preceptors will observe from a control room down the hall. Students will receive valuable feedback about their patient examinations from faculty preceptors and learn from watching the playback of their video/audio. As students advance through the curriculum, additional standardized patients will simulate particular illnesses.
Stacie Rearden Hall, an actress and a standardized patient for almost two years, noted that medical students are eager to learn from the perspective of a patient.
“Normally, they don’t get the opportunity to sit down with a patient after an exam to learn how well they communicated,” said Rearden Hall.
“I love this program. It’s a wonderful thing,” she said.
And the medical students are gaining valuable experiences learning to become not only highly skilled doctors but good listeners and communicators.
“It’s been really beneficial to hear what the standardized patients have to say,” said Allison Hastings, a second-year medical student who has worked with standardized patients several times. “It’s a really good opportunity for us to stop and think while it’s fresh in our minds. That opportunity for reflection and feedback is definitely important to improving our performance.”
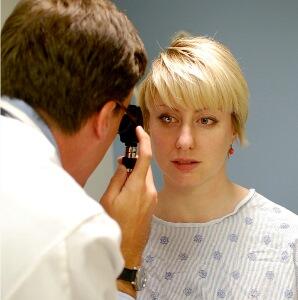
Arts and medicine collide
Anderson is no stranger to the arts-medicine collaboration. Since 2005, he has been working with colleagues in the VCU Schools of the Arts and Medicine to see how theater training could help physicians develop clinical empathy. In 2007, the VCU team published findings of a pilot study in the Journal of General Internal Medicine suggesting that doctors taught empathy techniques by theater professors show improved bedside manner. In 2010, that training transformed to become the VCU Standardized Patient Program, an in-house program offering services that were formerly outsourced.
“We started this idea by responding to what was then being called a ‘national crisis in health care’ – the technical side of medicine had grown so complex that humanism had been all but been pushed out of the curricula of many medical programs,” said Anderson.
In other work, Anderson works closely with David Leong, professor and chairman of the Department of Theatre, as well as Alan Dow, M.D., associate professor, and Richard Wenzel, M.D., professor, in the Department of Internal Medicine in the School of Medicine, to develop communication workshops that not only strengthen relationships between doctor and patient, but also between health professionals from various backgrounds working to heal a patient. This aspect is highlighted through interprofessional education – another key medical education innovation that has become part of the new curriculum.
“Teams of health care professionals need to communicate and be on the same page,” said Anderson. “We are working on skills and techniques to get them there.”
“Many times I’ve seen arts in medicine change a patient’s life … moments in health care are vastly important,” Anderson said. “Even miniscule changes can resonate a lifetime. All patients are vulnerable. This is the nature of health care. Arts in medicine can keep a terrible moment from being worse. It can make wonderful moments better. For an artist there is no higher calling.”
Subscribe for free to the weekly VCU News email newsletter at http://newsletter.news.vcu.edu/ and receive a selection of stories, videos, photos, news clips and event listings in your inbox every Thursday.
Subscribe to VCU News
Subscribe to VCU News at newsletter.vcu.edu and receive a selection of stories, videos, photos, news clips and event listings in your inbox.







