May 8, 2026
VCU biomedical engineer advances muscle regeneration technology
Share this story
Michael McClure still has a ways to go, but after more than a decade working on a novel regenerative therapy for severe muscle injuries, the Virginia Commonwealth University biomedical engineer says his team is closer than ever to bringing the trauma-repairing technology to human patients.
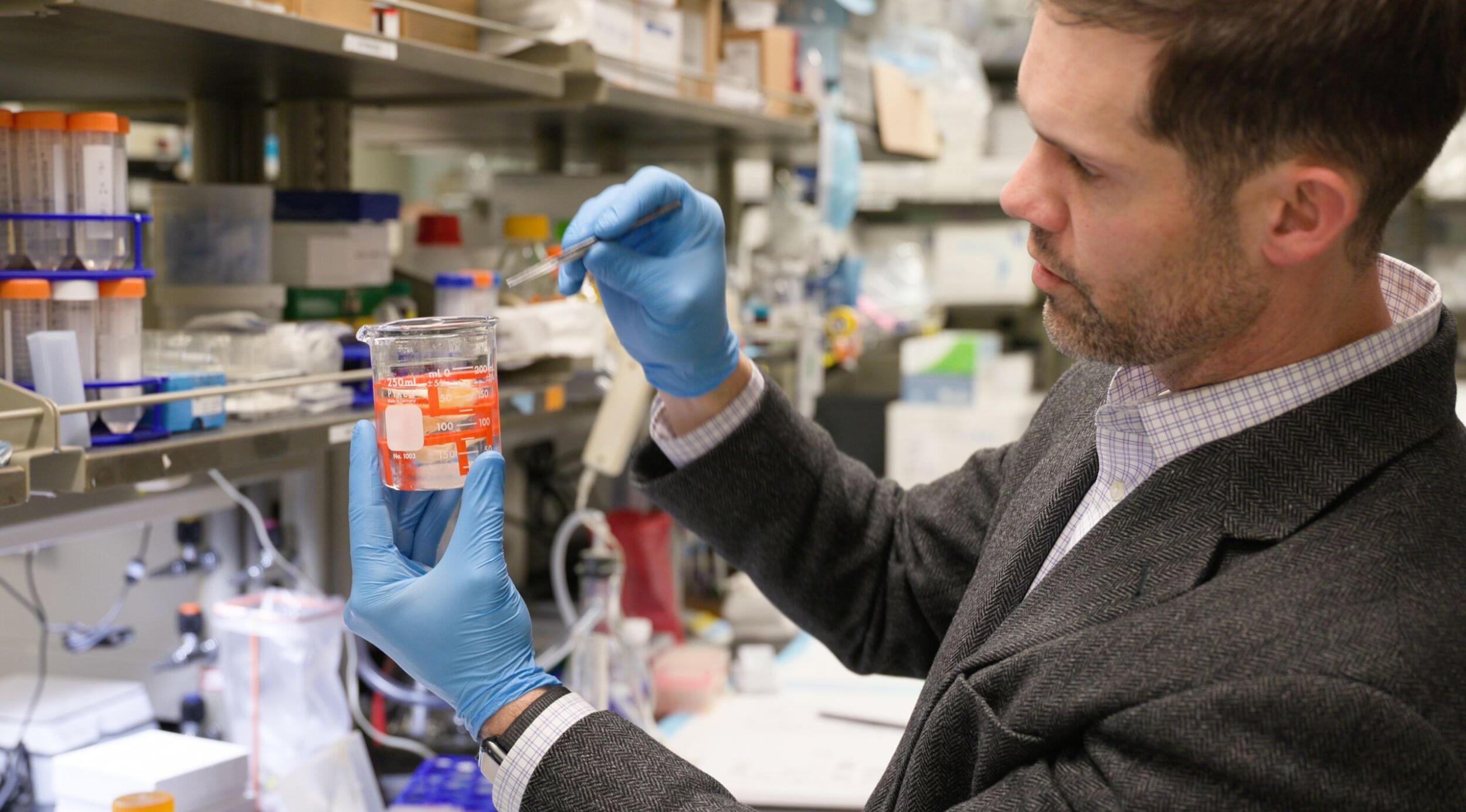
McClure, Ph.D., an associate professor in the College of Engineering’s Department of Biomedical Engineering, has been developing a method to regenerate muscle tissue lost to traumatic injuries. The approach relies on decellularization, a process that removes living cells from donor muscle while preserving the underlying biological structure that tells new tissue how to grow.
That structure, known as the extracellular matrix, retains the physical architecture and biochemical signals of muscle. Instead of transplanting foreign cells, the approach gives the body a blueprint it can use to rebuild tissue on its own.
“Decellularization is really just washing out the cells and leaving behind the scaffold that the cells were attached to before,” McClure said. “That scaffold becomes the regenerative product.”
If successful, the scaffolds could help people recover from devastating injuries that remove large portions of muscle, including blast injuries suffered in combat, car accidents and gunshot wounds.
“The goal is to implant these grafts into patients with severe muscle injuries and have them regenerate new muscle,” McClure said. “These are injuries where a significant amount of tissue is lost, and the body just can’t regenerate that on its own.”
He hopes the grafts will eventually be used to treat patients with volumetric muscle loss, a condition where the body cannot naturally regenerate enough tissue to restore function.
The research into the decellularized muscle matrix began around 2013, when McClure, then a postdoctoral fellow, started experimenting with ways to remove cells from muscle while preserving structure. By 2016, the research group was creating grafts, and over the years, it worked to improve its decellularization methods before filing for a patent in 2021.
Since then, the work has evolved through multiple rounds of refinement – from optimizing the chemical process that removes the cells to testing surgical techniques for implanting the grafts.
McClure’s work has been supported by the U.S. Department of Defense, the Virginia Innovation Partnership Corp. and internal funding from VCU, including commercialization support through VCU TechTransfer and Ventures and the Office of the Vice President for Research and Innovation.
That support – along with a push from mentor Barbara D. Boyan, Ph.D., executive director of VCU’s Institute for Engineering and Medicine – helped McClure take the next step. He formed a company, Sarcogenics, to move the technology closer to physicians and patients.
“I thought forming a startup was a crazy idea,” McClure recalled. “And then I thought a little more about it and realized that in order to actually make a real impact on medical devices and this industry for muscle injuries, I needed to form the company.”
The McClure lab’s opportunity is significant. The soft-tissue repair market is estimated at nearly $25 billion, with a U.S. scaffold technology segment valued at more than $600 million.
Today, the biggest frontier for Sarcogenics is not just regenerating muscle but reconnecting it to the nervous system. Without a functional nerve supply, regenerated muscle cannot contract or restore movement. That makes nerve integration, not just tissue growth, the key to restoring real function.
“We’re really excited about the connection of muscle and nerve together,” McClure said. “You have to reconnect that muscle to the nervous system. Otherwise, it’s not going to work.”
To address that challenge, McClure’s lab is studying techniques to introduce motor nerves into the grafted tissue – a process known as neurotization – and developing proteins that encourage the formation of acetylcholine receptor clusters on newly formed muscle fibers. Acetylcholine is the signal sent by nerves that tells muscles to contract.
The next phase is developing a human version of the graft and advancing toward preclinical and clinical trials – steps that could take five to 10 years before the first patient receives the technology.
For McClure, the long timeline is simply part of the process.
“The goal is to keep making improvements and keep getting to the next milestone,” he said. “You just keep pushing forward.”
Subscribe to VCU News
Subscribe to VCU News at newsletter.vcu.edu and receive a selection of stories, videos, photos, news clips and event listings in your inbox.










